In early 2019, the World Health Organization designated 2020 as the Year of the Nurse and Midwife, in honor of the 200th anniversary of Florence Nightingale’s birth.
The public health agency had no idea how prescient their designation would be.
Over the past 14 months, nurses — including UConn nurses — have responded to the call of duty to help fight the COVID-19 pandemic. From sacrificing their personal safety, to overcoming enormous demands at the bedside, or returning to the field if they are retired, nurses have bravely met this challenge.
In honor of National Nurses Week, which runs from May 6 to May 12 every year, the School of Nursing is recognizing its alumni for their hard work and dedication during the ongoing pandemic. Some go to work on the front lines every day, while others contribute to the fight through advanced studies and research.
We asked them to share their experiences from the past year with us, and know UConn Nation joins us in thanking them for all that they do:

Sophia Sopczneski ’10 (NUR)
The past year has definitely been the most challenging of my nursing career. Treating COVID-19 patients was unlike anything I had experienced, due to their level of acuity, the constantly evolving treatment plans, and the complexity of the illness.
I am proud to say my colleagues in the intensive care unit at The Hospital of Central Connecticut quickly adapted to the challenges of each new day and we are a much stronger team now for all that we experienced together. The photo I’ve included is of myself and another UConn alum from my class who coincidentally joined our team in New Britain at the beginning of the pandemic. We’re proud to be Huskies!

Sarah Harkins ’20 (NUR)
I’m a recent graduate, and I have been working in the Yale New Haven Hospital emergency room on the front lines of the pandemic for the past year. I’m a proud Husky and I’m thankful to UConn for preparing me so well! I’m now looking into graduate programs for next year.
Alexa Ben-Yishay ’19 (NUR)
Immediately following graduation, I worked as a registered nurse in labor and delivery at Holy Name Medical Center for a little over a year. I recently began a new job in the emergency department at St. Joseph’s University Medical Center, which is a Level I trauma center.
Going into clinical practice as a brand new nurse during the peak of the COVID-19 pandemic was very challenging. However, I believe all of my experiences have shaped me into the nurse I am today and have allowed me to drastically strengthen my clinical skills.
I will begin graduate school at New York University this coming fall to get my adult-gerontology doctor of nursing practice degree. I am looking forward to it!

Cynthia Heng ’09 (NUR)
After graduating from nursing school, I worked in the hospital setting for a few years before returning to graduate school to pursue my master’s. I worked in family practice for a few years before moving to Florida right before the pandemic started. This past year, I have been working in urgent care in Miami, where we have been mostly seeing COVID-related cases.
Amisha Parekh de Campos ’20 Ph.D.

Since graduating in May 2020, events have been a whirlwind. During the final writing of my dissertation and its defense, I had the honor of directly working with COVID-19 positive patients. Our palliative care team helped manage outbreaks and symptoms, assess patients, and use our expertise to work in an ever-changing environment.
In fall 2020, I was offered a joint position as an assistant clinical professor at the UConn School of Nursing and as the Quality and Education Coordinator at Middlesex Health, which was ideal to merge academic and clinical settings. Although navigating the pandemic was difficult, and starting a new position was challenging, I am so happy to have had the opportunity to use my skills and knowledge to work directly with patients and be able to share my experience with other clinicians and students.
Jayme Mandile ’18 (NUR)
I love working in the post-anesthesia care unit at Backus Hospital. The different range of patients, from ambulatory to critical care, keeps you on your toes and every day is extremely different regardless if the types of surgeries are the same.
Over the past year, due to COVID-19, our unit turned into a medical ICU to help support the rest of the hospital. It was a learning curve and stressful, but I tried to soak in every opportunity to learn something new. I was able to work alongside critical care nurses and tried to ask them as much as I could and learn from their experiences.
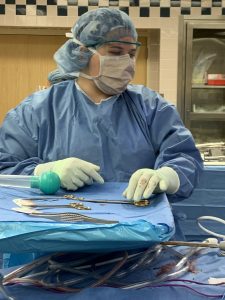
Samantha Marquardt ’19 (NUR)
I have been an operating room nurse at Yale New Haven Hospital since August 2019, and currently am a part of the transplant team handling kidney and liver transplants. I also circulate (and sometimes scrub into) all different types of surgeries, including robotics, vascular, general/trauma, cranio-maxillofacial, plastics, and thoracic. I have been able to get hands-on experience with Level I traumas, as well as be a preceptor to newer OR nurses.
From April to June 2020, I was sent to the intensive care units to be a member of the prone team. We would flip COVID-19 patients onto their stomachs to improve their oxygen levels. I saw the sickest of the sick during my nine weeks on the prone team.

Lucinda Canty ’20 Ph.D.
Over the past year, I have been sharing my dissertation research findings to address maternal health issues on a local and national level. My dissertation is titled “It’s Not Always Rainbows and Unicorns: The Lived Experience of Severe Maternal Mortality among Black Women.”
I am involved with initiatives that develop knowledge in the areas of diversity and racism in nursing. My experience in developing, initiating, and hosting the “Overdue Reckoning” project has provided deep understanding of what is required for an effective diversity, equity, and inclusion program. This unique initiative was launched in September 2020 to open discussions that focused on coming to terms with racism in nursing – a “reckoning” that acknowledges the reality and begins a process of healing and change.
The initiative featured five weekly Zoom discussions, in which between 110 and 120 nurses participated. In addition to the discussions, I met at least once a week with the co-leaders of the project, Peggy Chinn, Christina Nyariti, and Jessica Dillard Wright, to not only plan and debrief before and after each session, but also engage in our own process of reckoning with racism.
Our program resulted in a monthly support group for nurses and nursing students of color, a documentary film focusing on the experience of nurses of color (in development), a second discussion series for nurses which focused on the book “White Fragility,” and monthly Overdue Reckoning discussions. One of the most gratifying outcomes of this project is the ongoing support group that BIPOC nurses from across North America, the United Kingdom, and South Africa have formed, which includes retired nurses, nurses currently engaged in practice and education, students, and new graduates. The ongoing intergenerational support that has developed in this group is invaluable.

Mallory and Samantha Edrich ’20 (NUR)
My triplet sister and I became nurses together and are lucky enough to both work at UConn Health! I (Mallory) work on UT 3 and Samantha works in the emergency department. We loved being able to study and experience clinical hours with each other at UConn and now sometimes we even get to see each other at work! Despite the hardships of this past year, being able to become nurses together has been amazing and it’s all thanks to UConn!
Haley Meier ’15 (NUR)

I stepped into the charge nurse role for the day shift just before the pandemic hit and also found out I was pregnant with my first child.
My unit became the dedicated non-COVID unit and all pregnant/immune-compromised staff were sent to work there. This put me in charge of a whole new population with all new staff. It was a major learning curve, but fortunately we have since returned to our typical population and usual staff. I spent my maternity leave trying to get ahead in graduate school, so now I’m even closer to getting my doctorate in psychiatric nursing.
Maureen Groden ’90 MS

This past year has been the most difficult of my career. In March 2020, we faced the challenging task of finding enough personal protective equipment for our staff and the sudden departure of several psychosocial-spiritual staff members. As Director of Hospice and Palliative Care at the Holyoke Visiting Nurse Association, I had to guide, support and educate staff who were worried about patients, families, and their own health. Everything was changing and uncertain.
My office is right above the ambulance bay for the emergency room, and there were barely enough spaces for the ambulances to park. The managers and directors met frequently to review guidance from the Department of Public Health and the Centers for Disease Control and Prevention, as well as our own Valley Health System leadership and Command Center.
As the year went on, we negotiated nursing homes’ rules, tested staff every one to two weeks, became used to wearing PPE, and met remotely. We have survived surges, staff illnesses, and patient deaths. Nurses have been remarkable in their courage and dedication to people who are ill and dying. I am chair of the selectboard in my town, and we also faced PPE supply issues, residents’ illness and death, and held numerous meetings to provide residents with the knowledge and services they need to stay safe.
Meghan Wood ’19 (NUR)
I share my birthday with Nurses Day, and look forward to this day each year to reflect on my growth in my career and personal life. In the past year, I’ve completed my first year of orientation while working as a circulating registered nurse for congenital heart surgery at Boston Children’s Hospital. Each day, I’m more amazed by the strength of our patients and the incredible things they can achieve, despite the odds.
Raymond Blair ’20 (NUR)
After graduating, I became one of the first new grad nurses to ever be hired to the STAR Team at Hartford Hospital.

Being a full-time float nurse has given me a chance to learn how to function effectively on multiple different units, including COVID-19 units. While it was challenging to orient myself to multiple floors throughout the hospital, as opposed to one like most new nurses, it offered me the opportunity to expand my knowledge in multiple specialties, such as cardiology, neurology, and even emergency observation.
Kristen Biatowas ’17 (NUR)
It will be two years in July that I have been in my position as a mother baby nurse at Yale New Haven Hospital. At first, it was recommended that COVID-19 positive mothers be separated from their newborns at birth, though that has since changed.

I took care of one new mother who wore a mask and gloves when holding her new baby, which was difficult to see. I also cared for a COVID-19 positive mother of twins whose husband could not be at the bedside because he also had the virus. She was a new mother and not having her husband there was tough.
In addition to working on the mother baby unit, I also work at Yale University as a registered nurse. This past year, I was stationed in dorms giving flu vaccines to students. I also was able to see the incredible COVID-19 testing booths that were built in the dorms. When flu season started winding down, COVID-19 vaccines started ramping up. I was trained to give COVID-19 vaccines in December and it is amazing to be a part of the vaccination team at Yale.
UConn taught me that change is constant as a nurse. It has never been more true than this past year. Though the support from the community has been outstanding, self-care has been fundamental to being a nurse during this time.
Follow the UConn School of Nursing on Facebook, Instagram, Twitter, or LinkedIn.



