After a day of lifting heavy boxes, William “Bill” Poleshuk thought his back pain was a pulled muscle and was provided pain relievers by his primary care doctor. Although he initially had relief, the pain returned and his doctor ordered an x-ray. The x-ray showed a mass outside his right lung that had wrapped around his ribs, destroying one and fracturing three others.
He was referred to Dr. Omar Ibrahim, Director, Interventional Pulmonary at UConn Health, and a CT scan was performed. He was scheduled for a biopsy to see if the mass was cancerous, however ended up in the Emergency Department with the growth the size of a plum in his thigh that had seemingly grown overnight.
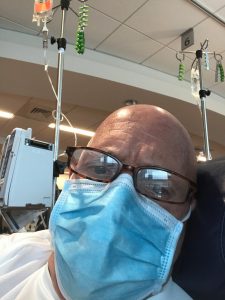
By then the cancer had moved to his lymph nodes even to his thigh. The tumor on his right lung was stage four, advanced non-small-cell lung cancer.
Advanced non-small cell lung cancer (NSCLC) is the most common type of lung cancer, with a poor prognosis and no known cure. Survival time is often short because of limited treatment options. Recent advances in targeted therapy and immunotherapy have changed the landscape for the treatment and prognosis of advanced NSCLC. Some may benefit tremendously, others not at all.
Poleshuk had been a smoker for 45 years and his sister, who also smoked the same brand for the same period of time had also been diagnosed with stage four lung cancer three months before him. He had been smoking two packs a day at the time of diagnosis and he quit smoking immediately.
He began his oncology treatment with Dr. Susan Tannenbaum, chief of the Division of Hematology and Oncology, Department of Medicine, and the section chief of the Carole and Ray Neag Comprehensive Cancer Center at UConn Health.
The cancer was moving quickly and he began to have other growths in his throat, tonsils, lymph nodes, and a new spot on his lung. The pain created by the tumor required heavy narcotics and he started radiation and completed ten rounds.
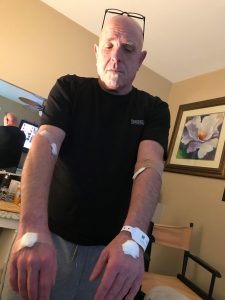
He started his treatment regimen in March 2020, with KEYTRUDA®, an immunotherapy that works with the immune system to help fight certain cancers.
The immune system is your body’s natural defense against disease. The immune system sends certain types of cells called T cells throughout your body to detect and fight infections and diseases—including cancer. PDL-1 is found on cancer cells and allows them to hide from the T-cells, the immune system, and maybe a cause for cancer growth and progression in some patients. Additionally, it is a marker for those who may respond to immunotherapy like KEYTRUDA. KEYTRUDA works by blocking the PDL-1 pathway to help prevent cancer cells from hiding.
KEYTRUDA helps the immune system do what it was meant to do: detect and fight cancer cells. Bill’s PDL-1 was 100%, extremely high, so he was an excellent candidate for the treatment. If tolerated and a good response is achieved, patients generally stay on the drug for two years based on prior studies.
Bill had been in a great deal of pain and continued on strong painkillers. He received only two treatments with immunotherapy when he began to be very tired with reduced appetite and profuse sweating.
“It didn’t feel normal, I was sweating through clothes for five hours a day,” says Poleshuk. “I couldn’t eat or drink and everything tasted terrible.”
He was found to have a less common side effect of the KEYTRUDA, immune hepatitis, a severe inflammation of his liver, responsible for his new problematic symptoms.
Poleshuk ended up in the hospital a few times for intravenous fluid for dehydration due to lack of oral intake. There was talk of giving him a port and another round of the KEYTRUDA, however, after meeting with Tannenbaum and Dr. Aswanth Reddy, a Hematology-Oncology fellow involved in his care, they decided to hold and monitor. He received only two treatments with his last at the end of April 2020.
“At that point, I was so worn out I told them that I didn’t want to do any further treatment until I could eat and drink again,” says Poleshuk.
In July he had a PET SCAN and the tumor was gone. He never received further treatment and his most recent CT scan on November 3, 2021, continued to show no sign of cancer; it appeared to be completely gone. Such responses are rare but illustrate the power of our immune system when unleashed by medications like immunotherapies. It impacted Bills’ normal tissues (in this case his liver) in addition to the destruction of his tumor. It is impossible to know if this will last forever, but for almost two years he has no evidence of cancer.
“Dr. Tannenbaum told me I was a miracle, that I really shouldn’t be here,” says Poleshuk. “The good Lord wants me to stay here.”
That with a lot of help from new medications used in the war against cancer, there is hope. For Bill, it was a combination of the tumor characteristics and his immune system that now almost two years after diagnosis, has given him a new lease on life.
Poleshuk didn’t work for a year and it took a while for his pain to resolve, however, he is now fully controlled off medications. He has returned to work full time but knows to listen to his body and rest when needed.
“During the time I was on my cancer journey, I lost several friends to lung cancer,” says Poleshuk. “I was never scared or thought I was going to die.”
He now encourages others to quit smoking or to never start, so they don’t have to go through what he did.
“If I can do it, anyone can,” says Poleshuk.



