Twenty-five percent of us are born with a PFO, or Patent Foramen Ovale, an opening in the heart between the left and right atrium which failed to close properly after our birth. As a result, this hole causes some blood to leak backwards from the right atrium to the left atrium.
While most of us never even know we have a PFO, some find out after a large blood clot formation passes through this tiny hole allowing it to travel to the brain causing a stroke.
When you have a stroke due to an unknown cause it’s called “cryptogenic.” Up to half of all stroke cases are considered cryptogenic, especially those occurring in younger patients. Often a PFO may often be the ultimate culprit.

Linda Peer-Groves, 55 of West Simsbury, is a young stroke survivor. She had a stroke on Sept. 3 and doctors at UConn Health helped her find out exactly why to help prevent a future stroke.
“I’ve always been so active and healthy so I was very surprised that I had a stroke. As a young person it’s been a very different and difficult experience having a stroke. I always thought strokes strike much older people,” she shared.
Turns out a diagnostic test at UConn Health’s Cardiac Catheterization Laboratory showed a PFO hole was inside her heart and Peer-Groves had no idea her entire life.
“I didn’t know I had a PFO,” shared Peer-Groves. This August during long airplane trips to and from British Columbia’s Queen Charlotte Island to see her daughter she most likely developed a deep-vein thrombosis (DVT) blood clot in her leg due to the air travel that eventually traveled through her PFO in her heart and then up to her brain.
“I’ve flown my whole life and never once had a problem,” says Peer-Groves who has lived previously in Southeast Asia including Cambodia, the Philippines, and India.
Two weeks after her return from Canada to Connecticut Peer-Groves started to experience some weird weakness feeling in her hand and foot just on the right side of her body.
“I knew I was having a stroke,” said Peer-Groves. “I always heard you should never ignore any body weakness and to act FAST to get to the hospital if you think you are having a stroke.”
She quickly received the clot-busting medication tPA at the Emergency Department of UConn John Dempsey Hospital, home to a 24/7 Stroke Center.
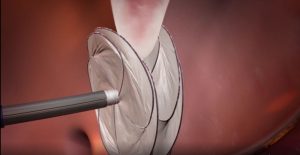
Once he discovered the PFO, interventional cardiology expert Dr. JuYong Lee, closed the PFO on December 13, 2021 minimally invasively via a guide wire placing a tiny device called Cardioform inside her heart to plug the heart hole between heart atriums forever and to prevent future strokes.
“Everything inside my heart now looks great! Now nothing can pass through my heart’s little hole thanks to this tiny heart device which looks like two umbrellas,” shared Peer-Groves who reports she didn’t feel a thing during the quick, same-day outpatient heart procedure performed minimally-invasively through groin vein access.
She is currently on aspirin and a blood thinning medication to reduce the chance of future blood clots forming as well. Plus, she is also continuing to make great strides during her physical therapy rehabilitation at UConn Health post-stroke.
“It’s been so encouraging. UConn Health is really helping me a lot,” says Peer-Groves who hopes her progress will help her return someday to being a French teacher once again in Bloomfield.
“My husband and I have a lot of confidence in Dr. Lee,” said Peer-Groves who is very thankful for his care and expertise.
“PFO closure significantly reduces the recurrent stroke risk compared to aspirin or blood thinning medical therapy alone in patients with cryptogenic stroke,” says Lee, director of vascular medicine and endovascular medicine and the non-invasive vascular laboratory, and interventional cardiologist at UConn Health’s Calhoun Cardiology Center.
Lee adds: “I am so happy to help patients like Linda actually know they have a PFO and help them prevent having a future cardiovascular event such as stroke.”



