A virus that was first found in sewers and shares its name – P22 – with a semi-automatic handgun might seem an unlikely object of beauty.
But to Carolyn Teschke, professor of molecular and cell biology, P22 is not only beautiful, it has absorbed her attention since she was a postdoctoral researcher in the early ’90s at MIT.
She recently was awarded a renewal of her $1.2 million National Institutes of Health (NIH) grant to study how P22 assembles itself, knowledge that could one day be applied to other, more complex viruses. Ultimately, this type of basic research could help identify ways for drugs to target viruses, such as those that cause the flu or common colds.
P22, which infects only Salmonella bacteria, might itself become an object of interest – and beauty – to more than microbiologists. As bacteria become more and more resistant to antibiotics, interest is renewing in phage therapy – using bacteriophages (viruses that attack bacteria) to combat infections.
While phage therapy was first popularized in the early 20th century, the discovery of antibiotics overshadowed it. Now that antibiotics are losing effectiveness, clinical trials are being done in the U.S. on using phages to treat wounds, among other things. In other parts of the world, such as eastern Europe, phage therapy has long been more popular.
Bacteriophages have also been identified as potential defensive weapons in bio-warfare.

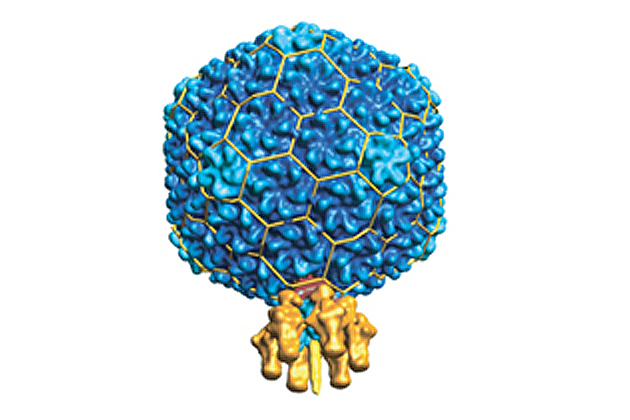
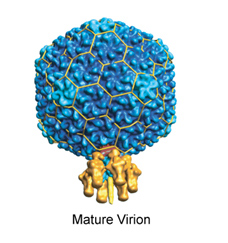
But Teschke’s interest in P22 is more basic. She wants to know how it forms its capsid, an outer shell of proteins that encapsulates its DNA. Each capsid of P22 has exactly 420 proteins – no more, no less – arranged in a sphere that is always the same size. It looks, Teschke says, like a perfect little soccer ball, only the inside contains genetic material.
“We don’t understand how the proteins know to do this,” she says. “And they generally don’t make mistakes.”
When P22 attacks Salmonella, its DNA takes over Salmonella’s own replication process to produce more of itself. Eventually, P22 overwhelms the Salmonella.
Viruses have a wide variety of shapes and sizes, all starting with a protein. Knowing how they form would help scientists understand how to inhibit their formation and how to design drugs to do this.
P22 has a simpler structure than viruses such as HIV or herpes, making it an ideal subject for study. All of its double-stranded DNA has been identified, and biologists know what all of its proteins do. They can mutate it and see what changes, knowing which protein caused the change.
In altering it, “We find the ones that don’t make the right things,” says Teschke. By mutating P22, they can force it to form tubes instead of spheres, or to make spheres of the wrong size, for instance.
“So we can get ideas about what parts of the capsid protein are important to determine size or shape,” she says.
“We are hoping that by understanding a very simple virus, we’ll be able to translate that understanding to a more complex one.”
That would include any virus that has a capsid – such as the adenoviruses that cause respiratory infections like the common cold. A capsid inhibitor could then halt the virus’s formation at an early stage.
“It’s definitely possible that we could someday develop a drug that would specifically inhibit a particular virus,” she says.
Teschke’s research group includes graduate students Maggie Suhanovsky, Alex Rizzo, Pauline Padilla-Meier, Molly Siegel, undergraduate Jonathan Novak ’12 (CLAS), and grad student Nadia D’lima.